2019 Blogs
12 of 80 items displayed

What the "toxic culture" at an NHS hospital reveals about how women experience the healthcare system
Clinical negligence solicitor, Rebecca Ridgeon, comments on what the maternity care scandal at the Shrewsbury and Telford Hospital NHS Trust reveals about how women experience the healthcare system.
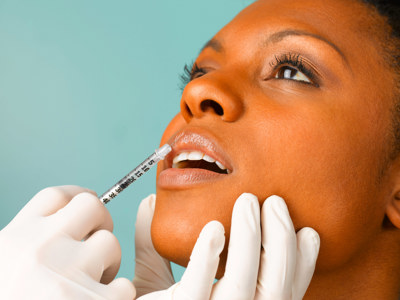
Safety over Glamour: The Dangers of Unregulated Cosmetic Procedures
Tina Patel from the consumer law and product safety team discusses the risks associated with cosmetic procedures and the lack of regulation in the industry.

Immigration detention – recent Supreme Court ruling will impact thousands
Human rights solicitor Waleed Sheikh discusses the importance of a recent Supreme Court ruling in relation to the approach by the Home Office to immigration detention.

Construction workers - worked to death?
Ross Whalley a lawyer specialising in injuries at work, examines the latest statistics from the HSE and asks why more isn't being done to improve safety where workers are most at risk, within the construction industry.

Trans Day of Remembrance 2019
Solicitor Alice Ramsay, from Leigh Day's employment department, discusses the importance of Trans Day of Remembrance

Peer on peer abuse guidelines leave too much to interpretation
With an increasing awareness that abusive acts can be carried out by children on other children, abuse claims solicitor Andrew Lord asks: is enough being done to safeguard children

Extinction Rebellion's Autumn Uprising: ERAU a month on
Gideon Habel revisits the issues for professionals wanting to show their support for the protests by Extinction Rebellion, following the High Court ruling, earlier this month, which declared the Met Police's section 14 Order unlawful

Food poisoning - more dangerous than you may think
Specialist food safety lawyer Angela Bruno discusses the impact food poisoning can have, with serious and potentially life-changing consequences

How to have a safe and happy Halloween
While the children are focused on the playful horrors of Halloween, the terrifying reality is that children's fancy dress costumes may neither be fit for purpose nor safe for wear.

A simple guide to the Human Rights Act 1998
You have probably heard the mention of ‘human rights’ somewhere in the media before. But have you ever learned the ins and outs of what the term truly means?

Are regulators watching Extinction Rebellion's 'Autumn Uprising'?
Gideon Habel of Leigh Day's regulatory and disciplinary team and Alice Ramsay of the firm's employment and discrimination department discuss the potential consequences for legal professionals in taking part in the ongoing protests by Extinction Rebellion.


