
Supporting Pneumoconiosis and Silicosis sufferers across the UK
Our Industrial Disease Team specialise in representing workers exposed to hazardous substances. We have successfully fought for compensation for individuals suffering from a range of occupational diseases.
Pneumoconiosis refers to a group of lung diseases caused by inhaling and retaining dust, resulting in lung tissue scarring (fibrosis). Silicosis, a prevalent form of pneumoconiosis, arises from inhaling silica dust, common in various industrial processes like cutting, drilling, and grinding.
Silica is a common, naturally occurring substance found in stones, rocks, clay, and sand as well as products such as bricks tiles, concrete, and some plastic composites. We specialise in silicosis claims representing miners, construction workers, sandblasters, and stone masons who have been exposed to high levels of silica dust. We have recently started to represent a ‘new wave’ of kitchen fitters exposed to silica whilst cutting artificial stone, also known as engineered stone.
A silicosis claim provides individuals with crucial financial support and can offer a sense of justice and recognition for the suffering endured because of exposure to silica dust in the workplace.
Compensation often helps cover medical expenses, lost wages due to inability to work, and ongoing care and medical treatment to alleviate the financial burden on families who may face significant challenges due to the impact of silicosis on the affected individual's ability to work and provide for their loved ones.
If you have been diagnosed with pneumoconiosis or silicosis, you may be eligible for compensation. Speak to our team today.
Watch our call to action to protect those who work with engineered stone
Silicosis FAQs
Silicosis is an irreversible lung condition caused by inhaling large amounts of silica dust over a prolonged period and poses significant health risks worldwide. Once inside the lungs, the silica dust particles are attacked by the immune system which causes inflammation and scarring of the lung tissue.
There are three types of silicosis. The length and extent of exposure to silica dust may determine the type of silicosis you develop.
- Chronic Silicosis occurs after prolonged exposure, typically over 20 years.
- Accelerated Silicosis develops after higher levels of silica exposure over 5-15 years.
- Acute Silicosis is less common but severe, resulting from brief exposure to high levels of silica.
Employees in various industries can face silica dust exposure and are at a higher risk of developing silicosis. You may have been exposed to silica dust working in the following industries:
- Construction
- Demolition
- Mining
- Glass manufacturing
- Paving
- Pottery and ceramics
- Sand blasting
- Stone masonry and cutting or fitting kitchen worktops
Common symptoms of silicosis can include:
- Shortness of breath
- Fever
- Fatigue
- Loss of appetite
- Chest pain
- Severe cough
However, silicosis can also increase the risk of developing other serious conditions. Lung cancer, tuberculosis, heart failure, kidney disease and chronic obstructive pulmonary disease are among the potentially life-threatening diseases resulting from silica exposure. There is no known treatment for silicosis as the lung damage cannot be reversed.
In some cases, people develop other diseases linked to silicosis such as scleroderma (affecting the skin or other organs), lupus and rheumatoid arthritis (sometimes called ‘Caplan’s Syndrome’).
Some people with silicosis have no lung symptoms at all, but may be prevented from working because they must not be exposed to dusty environments.
It is not always easy to diagnose silicosis as some of the initial symptoms can be quite vague and it is sometimes mistaken for other illnesses like sarcoidosis. If you are suffering with silicosis related symptoms and know that you have worked with silica dust or the products referred to on this page, it is important to visit your doctor and tell them that you worked in an ‘at-risk’ industry, as this is likely to be the best indication for them to identify whether silicosis is causing your problems.
If silicosis is suspected, your GP will refer you to a specialist lung doctor (a respiratory physician) for tests such as x-rays, lung function tests and CT scans.
Unfortunately, there is no cure for silicosis however there may be further steps that can be taken to reduce the risk of you developing further health conditions. Your treating doctors and nurses will be able to provide you with more information in relation to your treatment options.
The associated connection between dust and lung disease has been known for over a century. While health and safety protection in the UK has improved, which in turn has reduced the number of people developing silicosis, statistics from the Health and Safety Executive (HSE) shows that workers are continuing to be affected by the disease.
Recent events in Australia, where there has been a rise in cases of silicosis linked to the use of artificial stone in kitchen worktops, highlights ongoing concerns. Australia has banned the use of artificial stone due to silicosis cases, but the same material remains in use in the UK signalling potential future problems.
Chambers and partners 2024
The best in the field of industrial disease. They know exactly what they’re doing and are really impressive. They’re really easy to work with, very user-friendly and extremely switched on.
Bringing a compensation claim for silicosis
Employers have a duty of care to protect workers from health and safety risks, including silica dust exposure. Despite longstanding awareness, many workers still suffer. Our industrial disease lawyers help prove the legal relationship between workers and employers, securing compensation for their negligence.
Pneumoconiosis and silicosis compensation:
If you have been diagnosed with pneumoconiosis or silicosis, you may be eligible for compensation covering damages for pain and suffering, loss of income, past and future care, travel expenses, medical treatment, loss of services, loss of pension income, and other expenses.
For those at risk of developing more serious conditions in the future, provisional damages may be requested to allow for further damages to be claimed in future. This can provide the peace of mind of knowing that even if the worst happens, you or your family will be protected financially.
Access to State benefits:
The government has named silicosis and pneumoconiosis as “prescribed diseases” meaning you can claim State benefits if you are diagnosed. We can provide advice on where to get help with State benefits so you can obtain financial support while we investigate your claim.
Claims process:
Our specialist lawyers will gather evidence of your employment history, along with medical and occupational hygiene reports to support your case. Next, we’ll work to prove there was a “breach of duty” and that you worked in conditions which would have been deemed negligent at the time. We will also obtain medical evidence, usually from a respiratory expert, to confirm that your exposure to silica dust with your employer has caused you to develop silicosis.
If your previous employer is no longer in business, you can still claim against their old insurance company. We will go the extra mile to investigate and locate their insurers so that you can receive the compensation you deserve. Our team is here to support you throughout the process and fight for the compensation you are entitled to.
If you have been diagnosed with pneumoconiosis or silicosis, you may be eligible for compensation. Speak to our team today.
Our experience:
Our team understands the importance of seeking compensation as soon as possible and have had recent success in obtaining compensation for chronic, acute and accelerated silicosis cases. We are equipped to help prove that your employer had a legal duty of care towards you and breached that duty by exposing you to hazardous levels of dust.
Pneumoconiosis and silicosis case studies
“Leigh Day is the market leader that all other personal injury firms specialising in industrial disease look at with envy”
Legal 500, 2021
Recent news
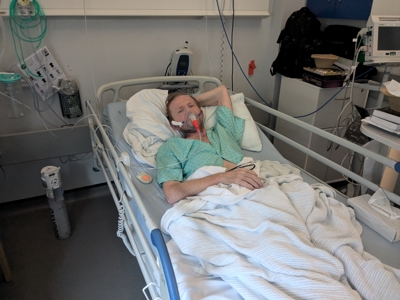
Stone worker with terminal silicosis says cutting quartz kitchen worktops in unsafe working conditions has cost him his life
A stone worker in hospital with terminal silicosis says he developed the disease after inhaling dust while cutting engineered stone, known as quartz, kitchen worktops in unsafe working conditions.

Stonemason quits job to “save his life” after being diagnosed with silicosis linked to working on engineered stone kitchen worktops
A stonemason from Ipswich, Suffolk says he had to quit his job to “save his life” after medical experts effectively warned that continuing to work with engineered stone, or quartz, could destroy his lungs.

Lawyers representing growing number of engineered stone workers with silicosis say tougher safety measures are urgently needed
Lawyers at Leigh Day, who represent a growing number of workers diagnosed with silicosis after manufacturing engineered stone kitchen worktops, say tougher safety measures are urgently needed to stop the rise in the deadly disease.
Blogs

Engineered stone and the rise of silicosis diagnoses
Ewan Tant, Partner, and Andrew Cooper, Senior Associate, explain what silicosis is and the dangers posed by engineered stone.

Lawyers representing growing number of engineered stone workers with silicosis say tougher safety measures are urgently needed
Lawyers at Leigh Day, who represent a growing number of workers diagnosed with silicosis after manufacturing engineered stone kitchen worktops, say tougher safety measures are urgently needed to stop the rise in the deadly disease.

